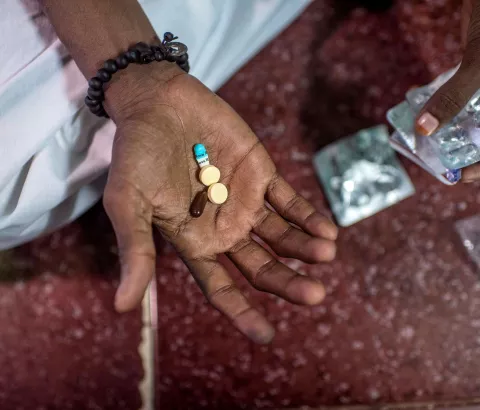
ANTIRETROVIRALS FOR HIV
Twenty years ago, the price charged for the triple cocktail of drugs to treat HIV was over US$10,000 for one person for one year, because of patent monopolies. Now, the same treatment is available for less than $100 per person per year, thanks to robust competition among generic drug manufacturers. This has allowed treatment scale-up from <1% of people with HIV in low- and middle-income countries having access to treatment in 2000, to 59% global
treatment coverage in 2017 (over 20 million people on treatment). However, we currently face access and innovation issues with child-friendly medicines, second- and third-line drugs for people whose initial treatment fails, and drugs for AIDS-related opportunistic infections. There are still too many people dying from this treatable disease!
THERAPIES FOR EBOLA
MSF has responded to Ebola virus outbreaks since the 1980s. Back then, the only thing our medical teams could do was isolate patients to stop the spread of infections and ease patients’ suffering until they died. No treatments were available at the time, which MSF highlighted starting in the late 1990s as the “fatal imbalance” in which only 1% of new drugs were for neglected diseases. When Ebola struck West Africa in 2014, this fatal neglect was made highly visible around the world – and MSF and others still had nothing to treat or prevent the disease. Now we have some promising vaccines and treatments undergoing testing, as well as new global institutions and funding focused on R&D of better tools to respond to outbreaks of Ebola and other emerging infectious diseases. But such collective responses must be supported and accelerated, and they must be held responsible for delivering lifesaving tools that are available and affordable for the people who need them most.
TUBERCULOSIS DRUGS AND DIAGNOSTICS
Despite recent advances in new drugs and diagnostics for TB, progress has been slow in scaling up treatment for people with the world’s leading infectious disease killer. In the past several years, two new drugs (bedaquiline and delamanid) and a powerful diagnostic testing device (GeneXpert) have become available, ending a decades-long gap in innovation. However, access and uptake of these new tools is lagging, as is continued R&D for faster, safer, simpler treatments for all forms of TB – including drug-resistant TB, which has become a major public health threat. Multiple political commitments have been made over the years, including the declaration of the first-ever UN High-Level Meeting on TB in 2018. But these need to be put into action. Governments have a collective responsibility to rapidly get many more people tested and treated, and to mobilise R&D and access to new tools.
HEPATITIS C MEDICATIONS
More than 70 million people worldwide have chronic hepatitis C virus (HCV) infection – but in 2016, only about 2 million people had received treatment. After many years of ineffective treatments, a breakthrough cure emerged – but at an outrageous price. In 2013, Gilead Sciences began charging US$1,000 per tablet for its new HCV drug sofosbuvir, while in 2015, Bristol-Myers Squibb started charging $750 per pill for its new drug daclatasvir. This resulted in a price of $147,000 per person for a single three-month treatment of both drugs! Following a similar strategy used for HIV drugs a decade before, MSF and civil society partners worked hard to overcome monopolies and seek ways to reduce the price of these drugs. In 2017, MSF announced it had been able to buy the same three-month treatment at a price of $120, allowing the scale-up of treatment in selected countries (along with simplified diagnosis and treatment protocols). However, in many countries, this treatment remains unavailable for the majority of people who need it – particularly in middle- and high-income countries, where companies continue to charge unaffordable prices that put a major strain on health systems.
SLEEPING SICKNESS CURE
Twenty years ago, MSF doctors needed to inject a potentially lethal arsenic-based drug called melarsoprol to save the lives of people with African sleeping sickness. The drug was so painful to receive, some patients called it “fire in the veins”, and so toxic that one in 20 patients died during treatment. MSF helped develop a better treatment called NECT, using a combination of existing medicines developed for other diseases, but it was still very cumbersome to use. Now, a new simple oral pill called fexinidazole has been developed and approved by our partner, the Drugs for Neglected Diseases initiative (DNDi). This new drug no longer requires patients to first undergo a painful spinal tap for diagnosis and is ready for use by people facing this deadly disease.